You’ve Been Told You Have a Heart Murmur. What Happens Next?
Introduction
It’s a moment that can stop you in your tracks. You’re at a routine check-up, perhaps for something entirely unrelated, and the doctor places a stethoscope on your chest. You expect to hear a reassuring “everything sounds fine.” Instead, they pause, listen again, and then utter the words: “You have a heart murmur.”
For most people, this is a confusing and often frightening experience. What is a heart murmur? Is it serious? What does it mean for my future? The internet, with its endless pages.
My name is Inderpaul Birdi, and I’m a cardiothoracic surgeon. For over two decades, I’ve dedicated my career to not just treating heart conditions, but to demystifying them for my patients. I founded The Keyhole Heart Clinic in London with a simple philosophy: to provide world-class care with a human touch. That means answering your questions, addressing your fears, and empowering you with the knowledge you need to make the best decisions for your health. This article is a part of that commitment.
We’re going to tackle the subject of heart murmurs head-on, in plain English, so you can move from a place of uncertainty to one of clarity and confidence.
What Exactly is a Heart Murmur? The Sound vs. The Cause
Let’s start with the basics. A heart murmur is simply an extra or unusual sound heard during a heartbeat. Think of it like this: the sound of a healthy heart is a steady “lub-dub, lub-dub.”
This is the sound of your heart valves opening and closing, directing blood flow in a smooth, one-way journey. A murmur is an additional sound, a “whoosh” or “swish,” that indicates the blood flow is turbulent or disrupted.
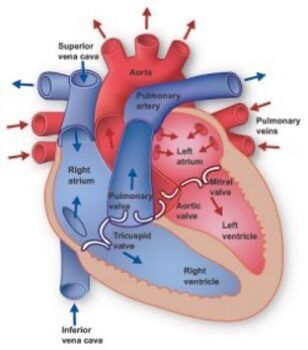
Figure 1: A basic diagram of the heart’s internal structure, showing the chambers and valves where murmurs can originate.
It’s crucial to understand that a murmur itself is not a disease. It’s a clinical sign, a clue that something might be happening inside your heart. We can categorise murmurs into two broad types:
Innocent Murmurs: These are common, especially in children and young adults. They are caused by blood flowing more rapidly than normal through a healthy heart. They are harmless and usually disappear over time. They don’t require any treatment or follow-up.
Abnormal Murmurs: These are the murmurs we pay close attention to. They are a sign of an underlying structural problem in the heart. This is where the sound isn’t the problem, but the cause of the sound is.
The Significance: Why You Can’t Afford to “Wait and See”
An abnormal heart murmur is often the first sign of an underlying issue that needs attention. While some issues are minor, others can be serious if left unaddressed.
The murmur is the body’s alarm bell, signalling that it’s time for a thorough investigation. For years, the standard approach to many heart problems was “watchful waiting.”
However, modern cardiology, supported by extensive research and guidelines like the UK’s NICE Guideline [NG208], has shown that this is often a flawed strategy [1]. By the time symptoms like breathlessness, chest pain, or fatigue appear, the heart may have already suffered irreversible damage.
Problems and Risks of Ignoring a Murmur
The biggest problem with heart murmurs is that they are often “silent.” You might feel perfectly fine while your heart is struggling to compensate for an underlying issue. This leads to several risks:
The “Wait and See” Trap: Many patients are told their murmur is “mild” and to come back in a year. But “mild” can become “severe” quickly, and without regular, high-quality monitoring, the window for the best treatment can close.
Misdiagnosis: Not all murmurs are created equal. A general practitioner might hear a murmur, but they cannot tell you why it’s there. Only a specialist with an echocardiogram can provide a definitive diagnosis.
Psychological Toll: Living with the knowledge of a “heart problem” without a clear plan is incredibly stressful. This anxiety can impact your quality of life more than the condition itself.
Comparisons – Which Test is Right for You?
When it comes to investigating a heart murmur, not all tests are equal.
ECG vs. Echocardiogram: An ECG looks at the heart’s electrical system. It’s useful but limited. An echocardiogram is the gold standard. It uses ultrasound to create a moving picture of your heart, allowing us to see the valves in action.
Stress Echo vs. Resting Echo: A resting echo is done while you lie still. A stress echo is done while your heart is working harder (via exercise or medication). This is crucial for patients who only experience symptoms during physical activity.
Cardiac MRI: This is used when we need even more detail about the heart muscle itself or when the echocardiogram images aren’t clear enough.
A Deeper Dive: Common Causes of Abnormal Heart Murmurs
An abnormal murmur is a sign, not a diagnosis. The sound is a clue that points to an underlying issue with the heart’s structure or function. Here are some of the most common culprits:
Heart Valve Disease: The Four Doors of the Heart
Your heart has four valves – the aortic, mitral, tricuspid, and pulmonary valves. They act as one-way doors, ensuring blood flows in the correct direction. When they don’t work properly, it creates turbulence, which we hear as a murmur.
Figure 2: The four valves of the heart. Issues with any of these “doors” can lead to the turbulent blood flow heard as a murmur.
Aortic Stenosis: This is a narrowing of the aortic valve, the final door blood passes through before leaving the heart. It’s the most common valve disease in the UK, often caused by calcium buildup as we age. When this valve narrows, the heart has to pump harder, eventually leading to heart failure.
Aortic Regurgitation: In this condition, the aortic valve doesn’t close properly, allowing blood to leak backward into the heart. This forces the heart to pump the same blood twice, leading to enlargement of the heart muscle and, eventually, heart failure if left untreated.
Mitral Regurgitation: This is the most common valve disorder, where the mitral valve, which separates the two left-sided chambers, leaks. It can be caused by age-related “wear and tear” or a condition called mitral valve prolapse. If left untreated, it can cause the heart to enlarge and lead to atrial fibrillation.
Mitral Stenosis: Less common in the UK now, this is a narrowing of the mitral valve, often a delayed consequence of rheumatic fever in childhood. It restricts blood flow into the heart’s main pumping chamber.
Tricuspid Valve Disease: Problems with the tricuspid valve on the right side of the heart often occur as a knock-on effect of left-sided valve issues. Tricuspid regurgitation can lead to significant swelling in the legs and abdomen.
Structural Defects: “Holes in the Heart”
Sometimes the murmur is caused by a hole in the wall (septum) that separates the chambers of the heart. These are often congenital, meaning they have been present since birth, but may not be discovered until adulthood.
Atrial Septal Defect (ASD): This is a hole between the two upper chambers (the atria). It allows oxygenated blood to leak back into the right side of the heart, causing it to do extra work. Over time, this can lead to enlargement of the right-sided chambers and rhythm problems.
Ventricular Septal Defect (VSD): A VSD is a hole between the two lower chambers (the ventricles). A large VSD will cause a very loud murmur and is usually detected in infancy. Smaller VSDs may not be found until later in life and can put a strain on the heart over many years.
Other Causes of Heart Sounds
Pericarditis: This is an inflammation of the pericardium, the thin sac that surrounds the heart. When this sac becomes inflamed, it can rub against the heart muscle, creating a distinctive scratching sound called a “pericardial friction rub.” While not strictly a murmur, it is an abnormal heart sound that can be detected during auscultation and requires investigation. Pericarditis is often caused by a viral infection and typically resolves with anti-inflammatory medication.
The Patient Journey: From First Call to Full Recovery
What does it actually look like to be a patient at The Keyhole Heart Clinic? We believe in transparency, so here is the step-by-step journey:
- The Initial Consultation: You meet with a senior consultant. We listen to your story, your symptoms, and your fears. We perform a physical exam and an ECG.
- The Diagnostic Phase: Usually on the same day, you have an echocardiogram. We don’t send you home to wait for a letter; we sit down with you and show you the images of your heart.
- The Decision: If treatment is needed, we discuss all options, from medication to manage symptoms to the definitive surgical solutions.
Treatment Options: From Medication to Modern Surgery
Once we have a clear diagnosis, we can create a tailored treatment plan. For many conditions, the first step is either observation over time, or medication. We might use drugs to control blood pressure, manage heart rhythm, or reduce the strain on the heart. However, medications can only manage the symptoms; they cannot fix the underlying structural problem.
When a valve is severely narrowed or leaking, or a hole in the heart is causing significant strain, surgery becomes the definitive treatment. This is where many patients become anxious, picturing the large scars and long recovery times of the past.
Cost of Investigation in the UK
One of the most common questions patients have is about the cost of investigation. In the UK, you have two main paths: the NHS and the private sector. The table below gives a simplified comparison.
| Service | NHS | Private (Typical) |
| Consultation | Free (wait list) | £250 – £500 |
| Echocardiogram | Free (wait list) | £285 – £600 |
| Wait Time | Weeks to Months | Days to a Week |
On the NHS, the care is excellent, but the system is under immense pressure. Waiting times for an echocardiogram can stretch into months. In the private sector, you are paying for speed and access.
At The Keyhole Heart Clinic, our Heart Health Assessment provides a comprehensive evaluation with a senior consultant, including an ECG and a detailed echocardiogram, often on the same day. This speed is not just about convenience; it’s about providing peace of mind and getting you on the right treatment path as quickly as possible.
The Evolution of Heart Surgery: From Invasive to Brilliant
To understand why we do what we do at The Keyhole Heart Clinic, you have to understand where we came from. For most of the 20th century, heart surgery was a very invasive procedure. To reach the heart, surgeons had to perform a “sternotomy” – literally sawing the breastbone in half and prying the chest open. While life-saving, the physical and psychological toll on the patient was sometimes immense.
I remember early in my career seeing patients struggle for months to recover from the trauma of the surgery itself, long after their heart had been fixed. They couldn’t drive, they couldn’t lift their grandchildren, and they were in significant pain. I knew there had to be a better way.
The Keyhole Revolution: Minimally Invasive Cardiac Surgery (MICS)
This led to the development of minimally invasive cardiac surgery (MICS), or what we call “Keyhole Heart Surgery.” Instead of breaking bones, we use specialized instruments and high-definition cameras to operate through small incisions between the ribs. It was a paradigm shift. We weren’t just fixing hearts; we were preserving the patient’s quality of life during the process.
Figure 3: A comparison between the traditional open-heart approach (left) and the modern keyhole approach (right).
| Feature | Open-Heart Surgery | Keyhole Surgery |
| Incision | 8-10 inch sternotomy | 2-3 inch side incision |
| Recovery | 3-6 months | 2-4 weeks |
| Pain | Moderate | Minimal |
| Scar | Large, central | Small, discreet |
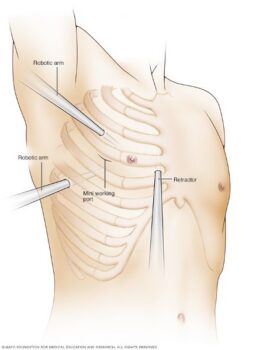
Figure 4: An illustration of the keyhole surgical approach to the mitral valve, showing how specialised instruments are used through small ports between the ribs.
Over the past 25 years I have performed keyhole heart surgery in nearly 2000 patients and I have seen the incredible recovery associated with these procedures.
In 2022, my team and I performed the UK’s first-ever quadruple heart bypass through a keyhole approach. And like all keyhole procedures this isn’t just about aesthetics; it’s about getting patients back to their lives faster, with less risk of infection and less pain.
Reviews and Expertise – Why Choose Us?
When it comes to your heart, you want the best. But how do you define “best”?
Experience: Look for a surgeon who has performed thousands of procedures and specialises in the specific technique you need.
Innovation: Choose a clinic that is at the forefront of medical technology, like The Keyhole Heart Clinic.
Transparency: A great medical team will answer all your questions – including the ones about cost and risks – openly and honestly.
When I founded The Keyhole Heart Clinic I was committed to becoming the best in the field, not just in the UK, but globally. We always combine surgical excellence with a patient-first approach that prioritises your recovery and your peace of mind.
Frequently Asked Questions (The “Unaskable” Questions)
Can I die from a heart murmur?
A murmur itself won’t kill you, but the underlying condition (like severe aortic stenosis) can be fatal if left untreated. The key is early diagnosis.
Can I still exercise with a heart murmur?
In many cases, yes. However, you must have a specialist assessment first to ensure that exercise isn’t putting dangerous strain on your heart.
Will I need surgery?
Not necessarily. Many murmurs are mild and only require regular monitoring. If you do need surgery, modern keyhole techniques make the process much less daunting than it used to be. It is very important to undergo tests to confirm the diagnosis AND to ensure regular followup to ensure that the cause of the murmur does not progress.
Is it my fault I have a heart murmur?
Almost never. Most valve problems are due to genetics, aging, or previous infections. The best thing you can do is take action now that you know about it.
Checklist: Preparing for Your Cardiology Appointment
To get the most out of your consultation, come prepared:
List of Symptoms: When do they happen? What triggers them?
Medical History: Previous surgeries, family history of heart disease.
Current Medications: Bring the actual boxes or a clear list.
Questions: Write them down so you don’t forget them in the moment.
Conclusion: Your Path to Clarity
Hearing that you have a heart murmur is the start of a conversation between you and your heart. It’s an opportunity to take control of your health before a small problem becomes a big one. At The Keyhole Heart Clinic, we are here to guide you through every step of that journey, from the first “whoosh” heard through a stethoscope to a full recovery and a return to the life you love.
Don’t let uncertainty hold you back. Reach out, ask the questions, and get the answers you deserve. Your heart is worth it.
References
[1] NICE. (2021). Heart valve disease presenting in adults: investigation and management [NG208]. National Institute for Health and Care Excellence. https://www.nice.uk/guidance/ng208
[2] British Heart Foundation. (2024). Heart Murmurs. https://www.bhf.org.uk/informationsupport/conditions/heart-murmurs
[3] The Keyhole Heart Clinic. (2026). Patient Outcomes and Surgical Data. https://khcdev.wpengine.com/outcomes
[4] American College of Cardiology. (2024). Guidelines for the Management of Patients With Valvular Heart Disease. https://www.acc.org/guidelines